 What Causes (PAD)?
What Causes (PAD)?
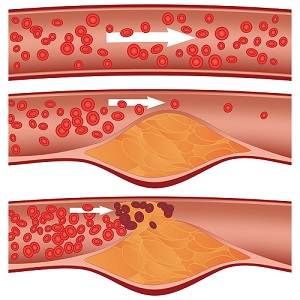
When a person is young, arteries are smooth and unobstructed but as we age arteries can become blocked through a process called atherosclerosis, which means hardening of the arteries. Atherosclerosis causes peripheral arterial disease (PAD).
A sticky substance called plaque builds up in the walls of arteries which consists of cholesterol, calcium, and fibrous tissue. As more plaque builds up, arteries narrow and harden reducing blood flow to the arteries in the legs, hips, buttocks, thighs, knees, shins, or upper feet causing discomfort, and pain when walking. It is important to treat this disease not only because it places a patient at greater risk for limb loss, but also for having a heart attack or stroke. It is entirely possible for a person to feel quite well and still have PAD or similar blockages in other arteries such as those leading to the heart or brain.
Stages and Symptoms
- Early Stage Many patients do not feel any symptoms from early peripheral artery disease. The most common early symptom is intermittent claudication (IC). IC is discomfort or pain in the legs that happens while walking and goes away when resting. Some patients experience tightness, heaviness, cramping, or weakness in the leg with activity. IC often occurs more quickly walking uphill or up a flight of stairs. Over time, the effects of IC can be felt at shorter walking distances. Only about 50 percent of the people with leg artery disease have blockages severe enough to experience IC.
- Moderate Stage Critical limb ischemia is the opposite of intermittent claudication (IC) where the legs do not get enough oxygen even when resting which causes a constant, throbbing pain in the feet or toes.
- Advanced Stage In severe peripheral artery disease, patients may develop painful sores on your toes or feet. If the circulation in your leg does not improve, these ulcers can start as dry, gray, or black sores, and eventually become dead tissue (called gangrene).
Risk Factors
People age 50+ are at increased risk of developing PAD, and men have a greater risk than women. There are other causes that relate to lifestyle or genetics that can be corrected or monitored to reduce risk including:
- Smoking
- Diabetes
- Weighing over 30% of ideal weight
- High blood pressure
- High cholesterol or triglycerides
- High levels of homocysteine in the blood (an amino acid)
If PAD is detected early symptoms can be managed and treated to prevent further damage or complication as follows:
- Quit smoking
- Manage diabetes by maintaining healthy blood sugar levels
- Maintain an ideal body weight
- Lower high blood pressure
- Lower high cholesterol
- Eat foods low in saturated fats and calories
- Exercise and walk regularly
Testing for PAD
There are a variety of tests used to determine the presence and severity of PAD. First, Dr. Tilara will complete a medical history, assess a person’s lifestyle, and conduct tests to measure pulse strength in the arteries behind the knees and feet. After the exam, if he suspects PAD, Dr. Tilara may perform tests such as:
- Ankle-brachial index (ABI) Used to compare blood pressure in arms and legs.
- Blood tests Checks cholesterol or other markers for artery disease.
- Duplex Ultrasound Uses high-frequency sound waves to measure real-time blood flow and detect blockages or other abnormalities.
- Pulse Volume Recording Measures blood volume at various points in the legs using an arm blood pressure cuff and a Doppler probe.
- Magnetic Resonance Angiography (MRA) Uses magnetic fields and radio waves to show blockages inside arteries.
- Computed Tomographic Angiography (CTA) Specialized CT scans and contrast dye is used to detect blockages inside the arteries.
- Angiography X-ray pictures of the blood vessels in the legs are taken using a contrast dye to highlight the arteries. Physicians usually reserve angiography for people with more severe forms of leg artery disease.
Treatment for PAD
- Medication: Most people respond well to lifestyle changes along with medication that controls cholesteral, high blood pressure, diabetes, and blood clots. Because each patient is different, no two treatment plans are alike. Dr. Tilara will put together a treatment plan for patients according to their unique symptoms and conditions that will improve the discomfort of PAD.
- Endovascular Treatment: Some people have advanced problems that require corrective minimally invasive endovascular treatment. The most common procedures include angioplasty, stent placement, and atherectomy.







